3D Brains
Much of the focus on postmortem human brains is (rightfully) keyed to what’s going on “under the hood”: the microscopic tissue changes, aggregates, and lesions which define neuropathological diagnoses. Yet significant insight can be derived from the macroscopic structural changes of the human brain in the settings of health and disease, including neurodegenerative diseases. “Gross pathology” has traditionally assessed and appraised the human brain using descriptive qualifications, subjective semi-quantitative scores, or imperfect structural proxies such as brain weight. In contrast, neuroimaging techniques eloquently capture, visualize, and measure longitudinal, structural changes of antemortem central nervous system (example: FreeSurfer). Postmortem ex vivo magnetic resonance imaging (MRI) is an excellent strategy for assessing brain structure as well as other cerebrovascular pathology (PMID 37955086 and PMID 39987858 are two examples from our brain bank and neuroimaging teams); however, access to MRI scanners and other technical resources can be limited for other brain banks or cost-prohibitive. As such, we have been interested in finding and developing other imaging modalities to assess brain structure.
Three-dimensional (3D) structured-light scanning can render high-resolution models of different objects using pulsed light and cameras. In our laboratory, we constructed a 3D modeling studio where we 3D scan every brain that comes into our brain bank. Why do we do this? Neurodegenerative diseases have “selective vulnerability” - certain neuronal networks or systems degenerate, while other networks/systems are spared. In turn, this results in tissue atrophy or shrinkage of specific brain structures. Measuring patterns of atrophy is important, especially when you consider the size and folding patterns (gyrification) of each individual brain is unique to begin with! The incredible value of these 3D brain models is threefold: 1) they improve our ability to work with the brain tissue (via 3D printed tissue matrices), 2) they can be analyzed to assess tissue atrophy, and 3) they are educational resources and references (especially when incorporated into augmented reality and virtual reality environments)!
To learn more about how we 3D model brains, check out our 2024 STAR Protocols publication.
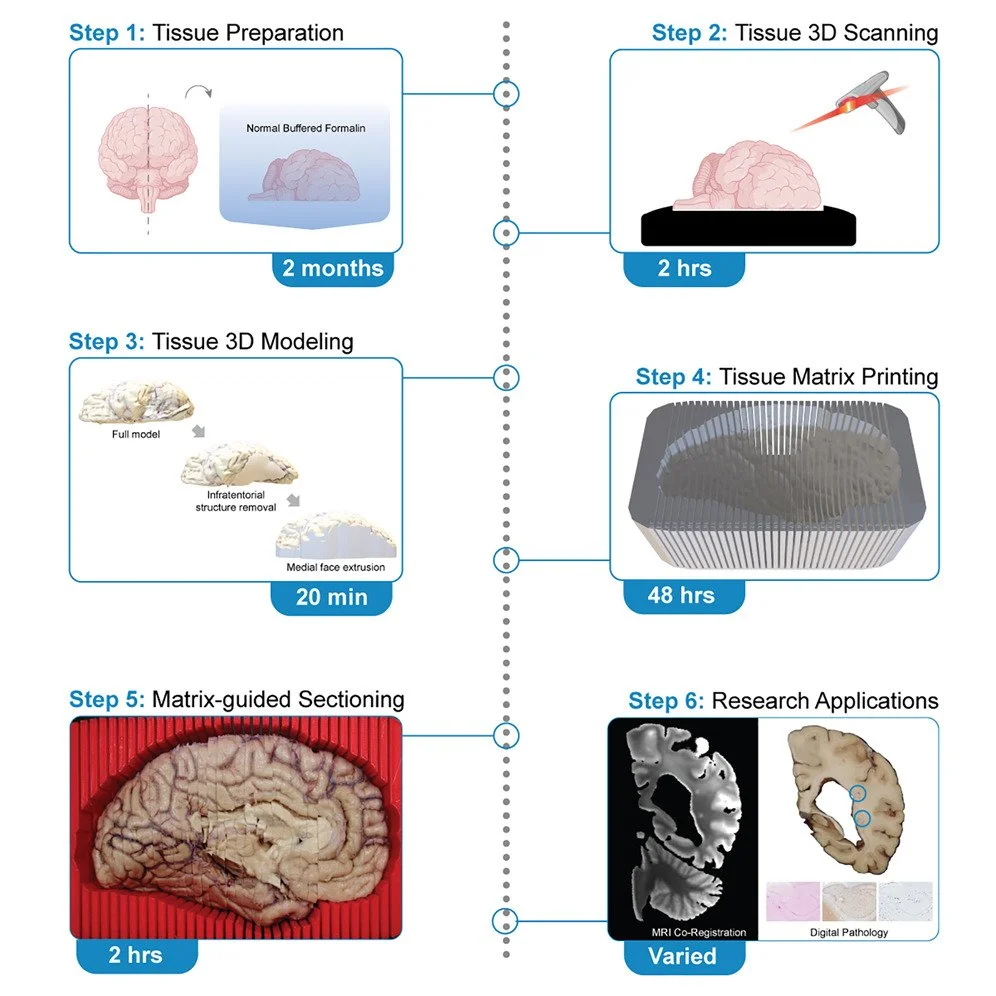
A tissue matrix is a container shaped to fit and snugly hold a specific structure, like a organ or tissue, for cutting that object in a precise orientation and thickness. Typically used for animal model research, matrices are uncommon in human brain research given the unique shape of each brain. Combining 3D modeling and 3D printing, we can create tissue matrices customized to the shape of each individual brain, cutting in the coronal plane, and at a thickness of 4 millimeters (the perfect fit for our tissue cassettes). These “brain cutting boxes” are made using polylactic acid (PLA) filament, take roughly 30-40 hours to make, and cost around $8-10 in filament. Cutting brains with a custom tissue matrix has several advantages: it makes brain cutting easier (removing technical, skill barriers), standardizes and streamlines cutting, minimizes tissue waste, improves safety (not having to hold in place while cutting), and when we’re done, serves as a container for organizing and storing the remaining tissue. Check out our STAR Protocols study to learn more!